With surgeries being canceled and postponed by COVID-19, clinics and hospitals collaborate and innovate to get through the pandemic.
On March 30 The Portland Clinic did not have any patients scheduled to meet doctors online. The next week, more than 400 online appointments had been made.
Dick Clark, CEO of The Portland Clinic, recalls a patient in her eighties who, in the past month, met her doctor during the first online video call of her life. “It warmed my heart to see the patient’s trust was still there,” he says.
In addition to connecting doctors and patients through telehealth visits, the clinic has had to postpone all elective surgeries, such as foot and ankle procedures, colonoscopies and tonsillectomies to prevent exposure.
While telemedicine visits have surged at the clinic since the outbreak of COVID-19, Clark says the clinic’s inability to perform as many surgeries has had a “devastating” impact on revenue.
“In-person visits have gone down 90% since the coronavirus outbreak,” says Clark. “We are projecting our revenue to be off 60% in April.”
The clinic, which employs 575 people, will furlough 180 employees in April and May, and has had to reduce staff hours to help with cash flow. The clinic has also closed two of its five locations.
Meanwhile, The Oregon Clinic has furloughed around 820 employees.
While hospitals nationwide will be eligible to receive at least $100 billion in financial aid as part of the federal government’s COVID-19 relief package, clinics can apply for loans under the Small Business Administration’s Payroll Protection Program, which is also intended to help nonprofits.
But mid-size clinics with more than 500 employees, such as The Portland Clinic, are not eligible.
“The good news is, we are expecting a surge of demand for health care beyond the COVID crisis,” says Clark, “But our clinics right now are on the brink of not being able to make it. There’s a gap in funding, and we are very fearful of that gap. We are unlike hospitals who are benefiting from federal support.”
Clark says that he has come together with CEOs from the The Oregon Clinic, the Oregon Medical Group in Eugene, The Corvallis Clinic and other medium-sized providers across the state to hire a lobbyist to advocate for the work provided by clinics.
“The hospitals need support. They do a huge amount of work, but we don’t want to be forgotten,” he says.
Clark began sharing information with his fellow CEOs remotely, and as they came together in conversation, Clark says that “momentum grew” to form a group to advocate for the needs of clinics at the federal level.
Hospitals have also had to scale back procedures to prevent exposure to the virus.
“About half of the procedures we’ve had to cancel or postpone have been elective procedures,” says Brian Terrett, director of public relations and communications for Legacy Health. “But the other half were procedures to help people with chronic conditions.”
The hospital system also closed its integrated medicine clinic and ophthalmology institute. Its weight and diabetes institute is only doing post-surgical visits and emergencies. “We figured the best thing we could do was just to put the information out in public as to what we were going to cancel.”
Terrett says Legacy Health has been able to benefit from sharing information with hospitals in Washington. “We heard from places in Seattle that they wished they would have started saving personal protective equipment before the virus hit, so we made sure to do that,” he says.
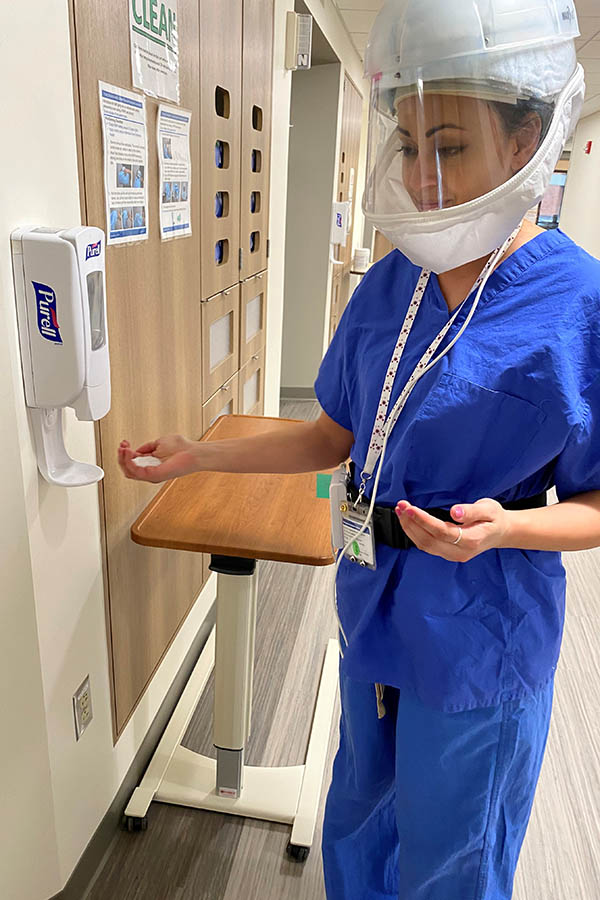
A Legacy Health worker hand-sanatizes. Photo: Legacy Health
“We’ve been able to learn from people who have had to deal with this thing before us. If a surge begins tomorrow, we are confident we have systems in place to be able to handle it.”
Legacy Health has also partnered with dental equipment manufacturer A-dec to provide protective masks to health care employees. It has also maintained a “robust” telemedicine patient care network.
As for the hospital system’s financial struggles, Terrett says that it will evaluate its position “once the dust settles.”
Rural hospitals and clinics also face a large burden from COVID-19. Senator Jeff Merkley, along with a bipartisan coalition of 18 of his Senate colleagues, sent an open letter to the U.S. Department of Health and Human Services to consider the special needs of rural hospitals when the department distributes federal funds. He argued that rural clinics are often the only choice for locals.
“Nearly one in five Americans live in rural areas, and depend on their local hospitals for care,” writes Merkley. “Prior to the COVID-19 pandemic, rural hospitals were already operating on shoestring budgets, and with the cancellation of elective procedures, have a desperate and immediate need for more funding.”
While the financial losses from COVID-19 could be existential threats to clinics and hospitals, Clark says Oregon health care will emerge from the crisis stronger and more connected than before. His clinic has since launched a joint fundraising effort with The Oregon Clinic, and other joint marketing opportunities are being discussed.
The collaboration between clinics will likely continue after the pandemic is over, he says.
“We’re in a category five hurricane right now, but I see all of Oregon health care emerging stronger after the storm,” he says. “If Oregon health care makes it through COVID-19, there are going to be tremendous opportunities. Video visits will be more commonplace. Our independent group will keep collaborating. We’re going to be stronger together after this.”
To subscribe to Oregon Business, click here.








