Share this article! Telemedicine, new partnerships and real estate diversification make health care more accessible in rural Oregon. Larry Mullins For putting hospitality into hospitals — literally The little town of Lebanon had a big weekend this June. Along with their iconic Strawberry Festival, which features marching bands, floats and the world’s largest strawberry shortcake … Read more
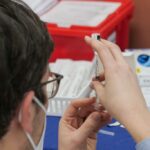
Telemedicine, new partnerships and real estate diversification make health care more accessible in rural Oregon.

Larry Mullins
For putting hospitality into hospitals — literally
The little town of Lebanon had a big weekend this June. Along with their iconic Strawberry Festival, which features marching bands, floats and the world’s largest strawberry shortcake parading down Main Street, residents also hosted the first graduating class of Western University of Health Sciences COMP-Northwest. The first new medical school in Oregon in 100 years, the facility is just one example of how Larry Mullins, CEO and president, Samaritan Health Services, is rethinking the assets and mission of rural health facilities.
16.9% of rural Oregonians live Sources: OHA Office of Health Analytics; |
Robust and convivial, the 65-year-old Mullins has reshaped the 54-acre Samaritan Health Sciences Campus to include the school, a conference center and an 84-room hotel with restaurants and bars. There are plans for apartments and retail on the site.
Located across the highway from Samaritan Lebanon Community Hospital, the campus represents Mullins’ approach to creating a financially sustainable future for rural health care. “We had all of this land that wasn’t producing income or value,” he says. “The idea was to build structures that would be beneficial to our health care mission and deliver a return back to the organization.”
Mullins has enjoyed success with this model before, adding fitness centers — including an in-house brand, SamFit — urgent care, pharmacies and offices to rural Samaritan campuses around the state. It’s a financial risk that private industry often isn’t willing to take. “We had a national fitness chain pull out in the 11th hour at our North Albany site, because they didn’t think we had the population,” he says. Mullins went ahead with a SamFit health club and reports hitting their membership goal in the first 90 days. Since opening in Lebanon in 2011, membership at the SamFit health club has increased tenfold.
The medical school, with approximately 400 students, conference center and hotel, offers a different synergy to the hospital and the community. Along with business and employment opportunities, the Health Sciences Campus might also solve the rural doctor shortage, which has reached critical proportions. “One-third of doctors stay in the state where they went to school; two-thirds stay where they had their residency,” says Mullins.

Ann Murray and Laurie Murray
For keeping the dream of the rural pharmacy alive
 Hard work. Connection to place. Extended families. It’s easy to romanticize life in rural Oregon. At first glance, Ann, 50, and Laurie Murray, 26, fit right into that tableau. This mother/daughter pair is part of the Murray family dynasty of pharmacists, with two small businesses in Heppner and Condon. A closer look reveals the struggle that threatens them and the communities they serve.
Hard work. Connection to place. Extended families. It’s easy to romanticize life in rural Oregon. At first glance, Ann, 50, and Laurie Murray, 26, fit right into that tableau. This mother/daughter pair is part of the Murray family dynasty of pharmacists, with two small businesses in Heppner and Condon. A closer look reveals the struggle that threatens them and the communities they serve.
The pharmacies were founded in 1959 and 1963, respectively, by Rod Murray. The Murray clan now includes seven pharmacists in the immediate family — including Sean, Laurie’s younger brother who graduates this year. Mother, father, aunt, uncle and grandfather all work in the two stores. Right now Laurie works for St. Anthony Hospital in Pendleton with hopes of eventually joining the family business. “I see myself part-time in Pendleton and part-time in one of the Murray locations.”
But will there be a family business left for her to join? Murray’s Drugs suffers the same affliction facing small business across America: competition from big chains. “Walmart can afford to lose money on their pharmacy,” says Ann, “but we can’t. Eighty percent of our revenues come from drug sales.”
The big bad wolves in this case are pharmacy benefit managers (PBMs), middlemen who dictate per-capsule payments for drugs. Sometimes PBMs set that payment at a loss for the pharmacy. Sometimes they bypass the pharmacy altogether, demanding that patients use out-of-state mail-order services.
Independent pharmacies across Oregon are fighting back, banding together to create buying groups to increase their power. Ann has taken the battle to Salem. She helped pass House Bill 2123 in 2013, which places restrictions on PBMs. She’s working on another bill for the short session in 2016 to give this law more teeth.
“Big chains will always beat us on price, but they can’t beat us on service,” says Ann. Laurie agrees. She says her family keeps cash prices for drugs low for people who want or need to pay out of pocket. “We know our clients,” she says.

Jim Rickards
For bridging the distance gap
Although radiology and dermatology seem like radically different health disciplines, they share a commonality: diagnosis from visual inspection. “Dermatologists visually identify problems 90% of the time,” says radiologist Jim Rickards, coordinated care organization health strategies officer for Yamhill County.
The global telemedicine market Source: BCC Research |
Worldwide revenue for telehealth Source: IHS |
The number of patients using Source: IHS |
The specialty is such a perfect fit for telemedicine that there’s already an app for it. Chicago-based Dermio is a direct-to-patient startup where users send secure iPhone pictures of their condition and consult with a dermatologist. Rickards partnered with Dermio to provide the same services to the Yamhill County CCOs.
As a radiologist, the McMinnville resident looks at pictures all day. As a health strategy officer, he sees the problems of rural Medicare and Medicaid patients seeking specialty treatment, particularly dermatology. “There is only one dermatologist for the 100,000 residents of Yamhill County,” he says. The number seems shockingly small but makes sense considering fewer than 400 new dermatologists are training to enter practice each year.
That scarcity makes it hard for anyone to receive care but extra difficult for the 25,000 residents who are on Medicare or Medicaid, which pay a lower rate for dermatology services. The result unduly burdens general practitioners who do not receive in-depth specialty training. “Dermatology pushes the limits of an internist’s training,” he says, “and sending people to Portland is challenging.”
Using a $15,000 grant from the Oregon Health Authority’s Council of Innovators, Rickards bought 15 iPad minis and trained one or two people per clinic as a “super-user” of the technology to manage the flow of data. “Snapping and sending a picture only takes five taps on the iPad, but managing a growing amount of responses, consultations and diagnosis is another matter.”
With the program installed in five clinics so far, Rickards reports some early wins. He sees telemedicine’s role expanding with more services, like identifying and treating diabetic retinopathy. “It can be difficult to attract doctors to rural communities,” he says, “but buying robust cameras and getting Wi-Fi is easy.”

Megan Haase
For substituting quality for quantity
Health care providers and insurers have traditionally used the fee-for-service model, billing for each doctor visit or test. Instinctual as that may be — what makes more sense than money in exchange for goods and services? — the system links health care compensation to volume of visits rather than quality of patient care. Mosaic Medical is one of three Federally Qualified Health Centers (FQHC) in the state trying something new: the Alternative Payment Model (APM).
The APM means that Mosaic is no longer financially bound to the number of patients they see. Instead they receive a per-patient monthly rate based on the size and composition of their patient population. “This allows more accessibility,” says Megan Haase, Mosaic’s CEO. “Now many needs are addressed outside of the traditional face-to-face clinic visit.”
Haase points to telemedicine, phone check-ins and remote monitoring as examples of what the APM model allows her staff to do. The model offers convenience and continuity of care to Mosaic’s rural patients in Madras, Prineville and Redmond where transportation is often an issue.
Put in place in March 2013, APM tracks patient and staff contact with metrics. The system is designed as a bridge to value-based pay, where providers are compensated based on overall population health. Laws and codes bar Haase from revealing how much per patient the state allocates Mosaic. But she says knowing the clinic’s monthly cash flow helps stabilize the operation. Haase also shares the challenges this experiment places on her and her staff. “It’s hard to find the bandwidth for these additional pilots and projects on top of our busy primary- care work.”
Trained as a family nurse practitioner and bilingual, Haase has been with Mosaic since its inception, starting at the Prineville clinic in 2002 and rising to CEO in the Bend location in 2010. Her journey allowed her to impact both individuals directly and the health system as a whole. “I knew I wanted to work with underserved communities,” she says. With Jefferson County ranked second from the bottom by the state in health outcomes, she knows her work is cut out for her. “This is an opportunity.”

Oliver Alexander and Orion Falvey
For not letting youth stand in the way
When Oliver Alexander and Orion Falvey founded Orchid Health in Oakridge in August 2014, they wanted to disrupt rural health care delivery. The recent University of Oregon graduates (emphasis on recent; Alexander is 23, Falvey is 24) hatched the idea while working on the school’s Social Business Challenge. The plan was a for-profit, subscription-based clinic, where patients paid a flat monthly fee for unlimited primary-care services.
The entrepreneurial pair found working examples of the model in San Francisco and Seattle. They opted to open in Oakridge, about 45 minutes southeast of Eugene, because 80% of the 3,500-member community’s primary-care needs were unmet. They received funding from a variety of investors who range from the town and county to crowdfunding to $100,000 from a private angel investor. They attracted a staff of eight, including a part-time doctor and a full-time nurse practitioner.
It didn’t work.
“I think the area’s lack of a middle class is to blame,” says Alexander. Undaunted, the two sharpened their pencils and pivoted their business plan, opting to serve Oakridge’s many Medicaid patients. “Seventy-five to 80% of the population is on Oregon Health Plan,” Alexander says.
They also added child and adult mental health to the clinic’s offerings, providing it both on-site and at area schools. “Mental health in school is a real innovation,” says Alexander. “As budgets get cut school nurses and counselors are the first to go.”
Operating for almost a full year, Orchid’s family practice is full with some 900 patients. The pair plans to add specialists and expand to other rural locations. “We have 22 sites in mind,” Alexander reports. They’re also on track to be profitable with a cash flow by the end of 2015.
Not that the pair is eager to get rich quick. Alexander states that he and Falvey, who grew up in rural Alaska, are dedicated to rural health. “Yes, we’re entrepreneurs,” he says, “but if we were in it for the money, we’d be on Wall Street.”

Brenda Johnson
For tearing down the walls
 Brenda Johnson discovered her mission in life after falling sick in Mexico as an undergraduate exchange student. “I accessed health care from physicians I didn’t know and in a language I didn’t understand,” says Johnson, chair of Jackson County’s coordinated care organization, Jackson Care Connect. “I made a vow at that time to ensure other people were cared for in a culturally respectful way.” In the United States, however, language barriers, socioeconomic factors and a fragmented delivery system create real road blocks to medical care. As chair of the CCO, Jackson is pulling those barriers down.
Brenda Johnson discovered her mission in life after falling sick in Mexico as an undergraduate exchange student. “I accessed health care from physicians I didn’t know and in a language I didn’t understand,” says Johnson, chair of Jackson County’s coordinated care organization, Jackson Care Connect. “I made a vow at that time to ensure other people were cared for in a culturally respectful way.” In the United States, however, language barriers, socioeconomic factors and a fragmented delivery system create real road blocks to medical care. As chair of the CCO, Jackson is pulling those barriers down.
Statewide 16 individual CCOs are trying this new way of delivering health care to the nearly 1 million members of the Oregon Health Plan, aka Medicaid. Launched in January 2013, Jackson Care Connect unites a network of health centers, addiction and mental health specialists, and dentists who work as a team to provide whole patient care while lowering costs. Like all CCOs, Jackson Care Connect is governed by a partnership of health care providers, community members and insurers. Just getting these three groups together in one room breaks new ground.
“I’ve never had conversations between clinical providers, insurers and consumers where everyone has equal power and say,” explains the 45-year-old Johnson, who is also the CEO of La Clinica, a network of community health centers. These discussions soften the once hard wall that divided these groups and reveal financial indicators, health outcomes and patient satisfaction for all to see.
They also reveal obstacles to care. For example, just getting to and from medical appointments can be a hardship for some clients. “That’s something healthcare providers knew little about,” Johnson says. Yet missed appointments often manifest into a crisis that requires a visit to the ER. As a CCO, Jackson Care Connect can now address nonemergent medical transportation and provide rides to those who need them.
Johnson, who has a B.A. in Spanish and nursing along with an M.B.A., credits Jackson County’s rural location with much of the CCO’s success. “Rural communities may not have as many resources to address systematic problems, but we have the advantages of relationships, which give us a more expansive understanding of root causes.”
Johnson admits that the more light they shine into the health care system, the more they find to fix. Still ,she knows that with the Affordable Care Act in place, the rest of the nation is looking to CCOs like Jackson Care Connect for ideas that can be transferred to other communities. “No question this is an improvement from before,” she says. “We’re still fragile, but this is too exciting to walk away from.”

Kathy Gunter and Deborah John
For getting kids out of the car and onto their feet
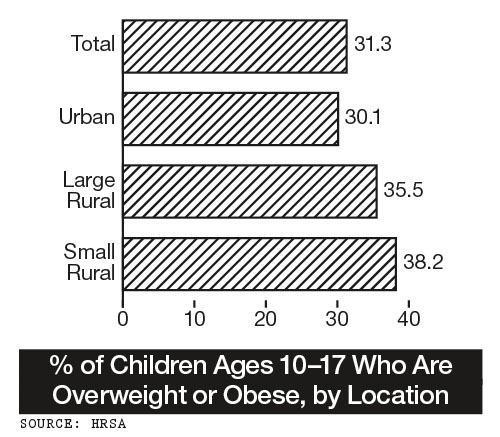 It’s not news that our sedentary, convenience food-laden lifestyle makes children fat, but it is surprising to learn that rural children have a 26% greater chance of being overweight than their urban or suburban counterparts. In fact, the definition of rural — great distances that are sparsely populated — exacerbates the problem. “In Oregon, 85% of rural children are bused to school, spending between 15 to 96 minutes sitting each way,” explains Kathy Gunter, an associate professor at Oregon State University’s College of Public Health and Human Sciences.
It’s not news that our sedentary, convenience food-laden lifestyle makes children fat, but it is surprising to learn that rural children have a 26% greater chance of being overweight than their urban or suburban counterparts. In fact, the definition of rural — great distances that are sparsely populated — exacerbates the problem. “In Oregon, 85% of rural children are bused to school, spending between 15 to 96 minutes sitting each way,” explains Kathy Gunter, an associate professor at Oregon State University’s College of Public Health and Human Sciences.
The distances make participating in after-school sports and activities difficult. Poverty and a lack of access to fresh food contribute to the problem. Bake in the lure of after-school screen time instead of outdoor play and rural Oregon becomes what the CDC calls an “obesogenic” environment where society itself promotes an unhealthy weight.
Gunter and her research partner, Deborah John, are leading a five-year, $4.8 million project funded by the U.S. Department of Agriculture to combat these issues. Generating Rural Options for Weight-Healthy Kids and Communities (GROW-HKC) builds innovative partnerships with the community, extension services and business in an effort to create significant, lasting change.
GROW-HKC kicked off by partnering with Corvallis-based startup GeoMobile Innovations. They trained parents and community volunteers to use the company’s GeoSnap photo inventory tool to document and map the environment, creating a visual database of resources for and barriers to healthy living.
“We found in Molalla there weren’t enough free resources to increase physical activity,” says John. So they partnered with the library, tourism board, contractors, and local writers and artists, and in May StoryWalk debuted. This literature and art installation, in which the pages of a children’s book are separated along a route, encourages families to walk and read together. GROW-HKC also helped create a series of trails in Clatskanie and fund a rock-climbing wall in Bonanza.
Gunter feels the combination of an engaged community and well-trained University Extension Services will create a broad base for preventive impacts after the project is over. “Our work is about prevention,” she says.

Erik Thorsen
For playing in the big leagues
Radiation therapy for cancer is a marathon of sprints. Individual treatments take only 15 to 20 minutes but must be administered every day for two to three weeks or longer. Inconvenience, disruption and fatigue are hard enough without adding a commute to the mix. Some 300 cancer patients on Oregon’s North Coast face that commute — either a 60-mile drive to Longview or a 100-mile trek into Portland. The situation is enough to make some patients contemplate abandoning treatment altogether.
Erik Thorsen, the 45-year-old CEO of Columbia Memorial Hospital in Astoria, found a solution by partnering with OHSU’S Knight Cancer Institute to create the CMH/OHSU Cancer Care Center. When completed in early 2017, the 18,000-square-foot, $10 million-plus center will offer 10 chairs for infusion treatments as well as imaging, pharmacy and other services.
This isn’t Thorsen’s first partnership with OHSU. In 2010 he helped create a cardiology clinic with the hospital. He understands the importance of collaboration. “Columbia Memorial is a private, nonprofit independent hospital with no government affiliations,” says the Warrenton native. “It’s tremendously challenging for a small, rural hospital to stay abreast of medical advancements and minimize administrative burdens without a partner.”
The alliance doesn’t mean that OHSU will swallow Columbia Memorial, Thorsen emphasizes. “I told my board that we’re rewriting the definition of affiliation. This is a clinical integration that’s self-sustaining for both entities. We are not financially joined at the hip.”
Funding for the clinic comes from three sources. Columbia Memorial, with its $85 million budget, will provide half while its foundation will give 25%. OHSU plans to fund the remaining quarter. Thorsen is hopeful that OHSU’s commitment and cachet will help recruit and retain highly skilled health care providers to the rural North Coast. He’s also hoping to attract a reverse commute in which Portlanders elect to have their cancer treatments as part of a coastal getaway.