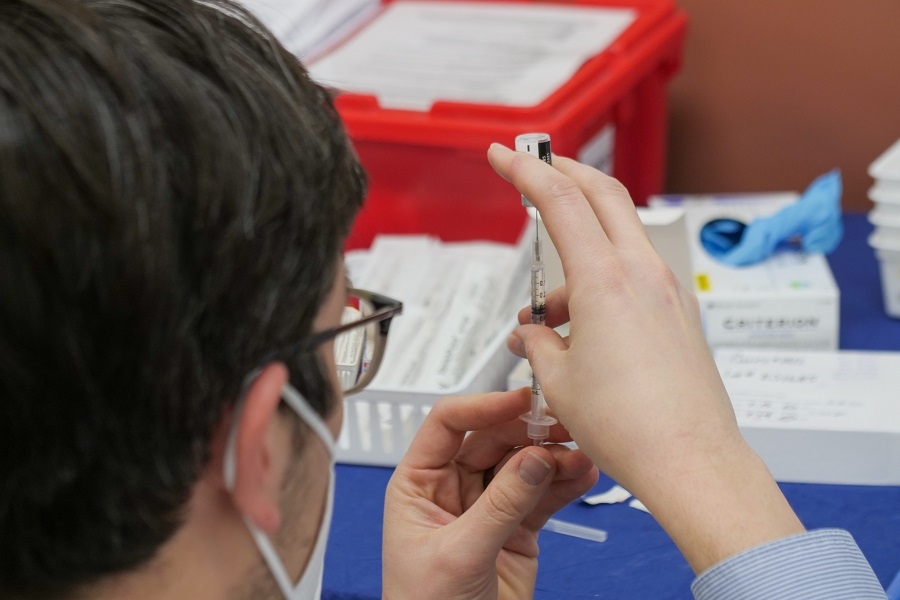
Businesses touted as solution to distributing COVID-19 vaccines.
On May 15 Oregon’s COVID-19 vaccination strategy was dictated by Operation Warp Speed, the Trump administration’s vaccine plan. Although the plan distributed vaccines to states quickly, it lacked state-level guidelines and distributed fewer doses than promised.
State officials and health care providers were put in a precarious position of having to decide how to distribute a limited amount of vaccines. Some health systems prioritized vaccinating their own employees before the most vulnerable people in the community.
“I wish there were more to Operation Warp Speed than ‘get the vaccine to the states,’” says Joe Ness, chief operating officer at Oregon Health and Science University. “A lot of granular details of the vaccine rollout were not considered.”
One month ago, the Biden administration set a more aggressive tone for dealing with the pandemic. Steps included committing $20 billion in defense funds to speed up vaccine manufacturing and distribution, assigning the Federal Emergency Management Agency to assist state agencies in setting up vaccination sites, as well as offering federal reimbursements to states that deploy the National Guard to help with vaccination clinics.
Despite encouraging numbers, demographic disparities and limited supply of vaccines and health care workers remain persistent problems in the fight against COVID-19.
Private institutions have already begun to shoulder some of the burden and make up for blind spots in the state’s vaccine distribution model. If businesses prove effective in bridging demographic divides, more private-sector solutions could be on the horizon.
RELATED STORY: Future of Work: Remote Working Saves OHSU Money and Space
Mass vaccination sites have already been set up across the state. Four of the state’s largest health care systems rented the Oregon Convention Center with the goal of providing 2,000 vaccinations daily.
Fairgrounds in Salem and Polk County have also opened as mass vaccination sites for eligible recipients, which include teachers, health care workers and the elderly. According to the Oregon Health Authority, 10% of Oregon’s population has already received a dose of the COVID-19 vaccine.
While the numbers show progress, demographic disparities remain a persistent problem in the state’s vaccine rollout. People of color and rural communities have not only been disproportionately impacted by coronavirus but also receive fewer doses of the vaccine per capita.
Hispanic communities, for example, have received roughly 5% of the state’s distributed vaccines, despite accounting for nearly 30% of overall cases, according to Oregon Health Authority data.
Despite this, people of color are not among the prioritized groups eligible for the vaccine. Gov. Kate Brown’s 27-member advisory committee cited the potential unconstitutionality of using race as a deciding factor in priorities groups.
“We say we want to get vaccines to the people who are most exposed and most at risk, but Black, Indigenous and other communities of color are being disproportionately impacted by the disease and given less access to the vaccine,” says Kevin Mealy, communications manager for the Oregon Nurses Association. “We have a situation where the problem and the solution are both increasing health disparities.”
Additionally, rural communities with less access to hospitals have much lower vaccination rates per capita than urban communities.
“We generally have enough nurses statewide but rural and remote areas often have a difficult time attracting health care providers,” Mealy adds.
For this reason the Oregon Health Authority took racial and demographic disparity into account when it distributed 100 vaccines to each of 127 retail pharmacy locations across the state. Pharmacies were chosen using Centers for Disease Control and Prevention’s COVID-19 vulnerability index, which prioritizes vulnerable communities, including rural areas and communities of color.
One of the companies that received doses was Fred Meyer. While the superstore chain was selected for its ability to immunize underserved communities, its effectiveness is constrained by the amount of doses provided by the state.
“Distribution is now at the county level. We are working with county officials to get vaccines to our stores as quickly as possible,” says Jeffery Temple, director of corporate affairs for Fred Meyer Stores. “We do not know when and how the county will be increasing the supply.”
Private pharmacies are also effective vaccine distributors since they do not tax the state’s already limited supply of nurses, many of whom are experiencing burnout.
“There was a national nurse shortage even before COVID-19 hit. The entire country needs nurses right now and there simply aren’t enough to go around. When we’re all drawing from the same shallow pool, it empties quickly,” says Mealy.
“Oregon has enough nurses today, but we may not tomorrow and there are many communities — particularly in rural Oregon — that already face provider shortages,” he says.
Mealy suggests allowing nursing school students to take part in vaccination clinics as a potential solution, as well as better funding for the state’s public health system. In the short term, however, pharmacies and large employers have the potential to close the gaps in care, provided they receive enough doses.
Employers could also advocate for mass employee vaccination clinics when more doses are received in the coming months.
Onsite vaccination clinics are already in place, but only for health care workers and firefighters. The model could be used to vaccinate grocery store workers, who are already at greater risk of COVID-19 exposure.
“Eventually, employers might need to have a hand at mass vaccinations,” says Ness. “Everyone is going to be required to do at least some part of this.”
To subscribe to Oregon Business, click here.