A Portland “TelAbortion” study is part of a sweeping digital health revolution that could upend the politics of abortion and contraception.
A groundbreaking study allowing women to get abortions via video is underway at the Columbia Willamette affiliate of Planned Parenthood (PPCW).
The “TelAbortion” project, part of a five-state initiative, works like this: A woman who wants to end her pregnancy consults with a clinician by video from her home. She gets an ultrasound, and the clinician reviews the results. If the woman is eligible, the clinician mails her FDA-approved medical abortion pills, then follows up by phone or videoconference.
The first Oregon participant was from a rural part of the state, where abortion clinics are more difficult to access, says Anne Udall, PPCW’s CEO. “It is probably a game changer.”
Reproductive health is back in the political spotlight.
An Oregon measure that would restrict public funding of abortion is on the November ballot, and abortion has become a central issue in the gubernatorial race between Gov. Kate Brown and Rep. Knute Buehler.
Pro-choice and anti- abortion groups are mulling the possibility of two Trump appointees to the Supreme Court, and a recent Supreme Court ruling determined “crisis pregnancy centers” in California cannot be required to tell their patients about the availability of abortion.
But if policy seems to revolve around restricting access, innovation around abortion and contraception services is moving in the opposite direction. Scientific developments are making contraception and abortion more readily available, and changes in the financing of contraceptive research are drawing more startups to the space.
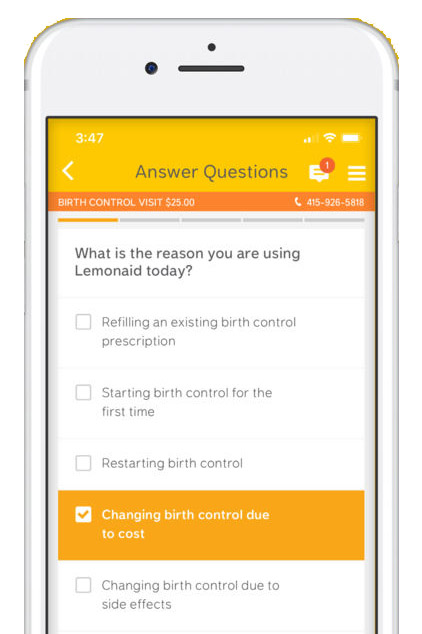
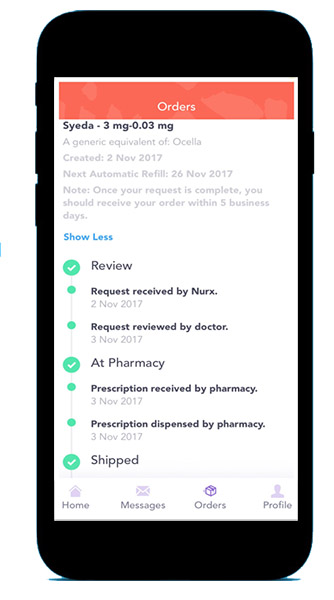
Telehealth is also changing the game. Nurx, a San Francisco-based startup that landed $36 million in venture funding last month, is one of several Uber-style platforms that bypass a traditional doctor or pharmacy visit to deliver birth control to your door. Lemonaid, another San Francisco startup, delivers birth control pills, patches and rings to customers in 23 states.
Digital technologies, of course, can be used to achieve multiple objectives, and groups on both sides of the reproductive-health divide are seizing the opportunity and sounding the alarm. Pro-choice advocates like Udall view TelAbortion as a game changer. But so does Lois Anderson, executive director of Oregon Right to Life.
Anderson points to medical abortion pills and telabortion, as well as insights gleaned from ultrasound, to bolster demands for policy change.
“We would argue that the entire structure of Roe is based on a medical-technology foundation that pretty much doesn’t exist anymore,” she says.
About three years ago, Dane Forst, a Portland graphic designer, was tooling about on the internet when he came across what he describes as a ”kickstarter-like” call for funding of a male contraceptive called Vasalgel, an injectable that would temporarily block sperm development.
“I had been wishing, hoping, reading for a few years about an eventual pill,” says Forst, 34. “So I thought: ‘I’m going to donate some money to this thing.’” (A sidebar on male contraception appears at the end of this article.)
Money drives innovation, and financing for contraceptive research has historically come from large pharmaceutical companies.
But in recent years, there’s been tremendous divestment by large corporations in the contraception arena. A 2010 review by the Gates Foundation estimated that donors from developed countries committed $85 million annually toward the global contraceptive technology pipeline, down $39 million from 1980 levels.
A high bar for safety is one reason drug companies have pulled out. Just last month, the pharmaceutical giant Bayer announced it will halt sales of its controversial Essure birth-control device in the United States at the end of the year, following reports the product had created scores of health problems.
“Contraception is so thorny,” says Jeff Jensen, vice chair for research for OHSU’s ob/gyn department and the director of the university’s women’s health research unit.
“While it’s universally used in women, and women benefit greatly from being able to voluntarily control their fertility, we see this tremendous social anxiety about it that is driven in large part and merged with the Republican party as a theme, that contraception services shouldn’t be publicly funded and that abortion should be eliminated.
“Then you have well-meaning progressives on the other side who think about the individual, who say: ‘Somebody may have been harmed, and maybe this is related. And this big bad company is making money off of this product.’ So the trial attorney pockets half a million along the way.”
 The gap left by pharmaceutical companies is opening up more opportunities for startups. Vasalgel, for example, is the brainchild of Revolution Contraceptives, a social-venture biotech company that itself is supported by the Parsemus Foundation, a nonprofit that targets medical research in neglected areas.
The gap left by pharmaceutical companies is opening up more opportunities for startups. Vasalgel, for example, is the brainchild of Revolution Contraceptives, a social-venture biotech company that itself is supported by the Parsemus Foundation, a nonprofit that targets medical research in neglected areas.
The National Institute of Child Health and Human Development/National Institutes of Health (NICHD/NIH) is funding multiple contraceptive development startups through its small-business grant program, according to Daniel S. Johnston, chief of the agency’s contraception research branch. Recipients in 2018 included Chapel Hill, North Carolina-based Eppin Pharma Inc.
The company launched in 2014 and last April published a paper on the results of its proof-of-concept study in OHSU’s Primate Research Lab.
Jensen himself is seeking investors to support a nonsurgical permanent contraception method that he hopes will revolutionize contraception, especially for women in developing countries.
The technology involves an injection of polidocanol foam, an FDA-approved treatment for varicose veins, in conjunction with another agent that Jensen declines to disclose, to trigger scarring in the fallopian tube and block conception.
“People say, ‘Contraception is a solved problem,’” says Jensen, citing another reason drug companies have abandoned the space. “That is not the case.”
Related Story: A conversation with Jeff Jensen, director of OHSU women’s health research unit
The problem is especially acute in parts of the world where women enter (or are coerced) into relationships at an early age. Many women in India, for example, have had several children by their early 20s, and then face several decades of unwanted fertility. “That’s where permanent contraception comes in,” Jensen says. “Many women don’t want to have hormones; they don’t want to have devices. They want simply not to have the risk of pregnancy.”
His polidocanol project is funded by a $6 million grant from the Gates Foundation, and he hopes to partner with the foundation for continued funding to bring the research into a Phase One clinical trial.
A landmark event occurred in the digital contraception space earlier this month, when the U.S. Food and Drug Administration approved the first “contraceptive app” designed to track fertility and prevent pregnancy. The Natural Cycles platform was part of the agency’s new Digital Health Innovation Action Plan, a program that accelerates approval for new low- to moderate-risk devices.
Launched in Sweden in 2014, Natural Cycles is already steeped in controversy. App or no app, critics say, family planning is hardly a foolproof way to prevent pregnancy.
At least 37 women have become pregnant while using Natural Cycles, which was designed by physicists and uses a complicated algorithm to improve on traditional fertility-tracking methods.
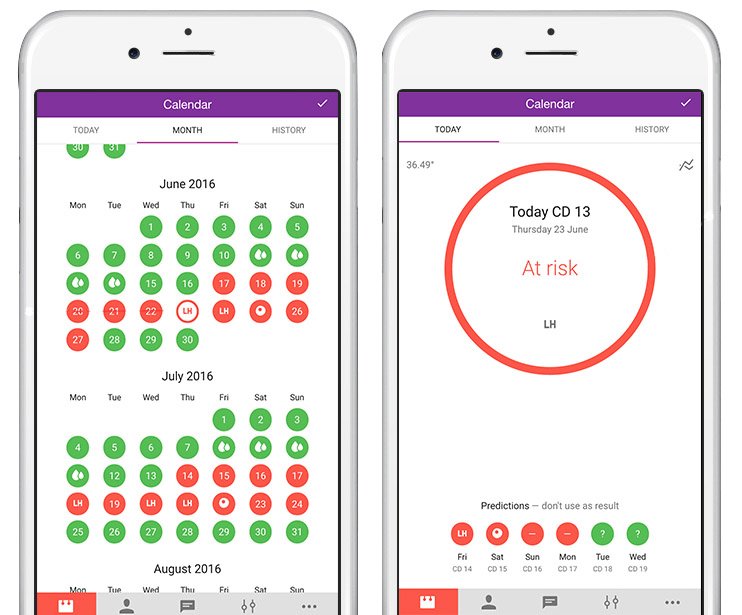
Regardless, the FDA’s approval marks the steady march of digital health models into the thorny world of reproductive health.
Spot On, a Planned Parenthood app, syncs ovulation to birth control methods. Lemonaid mails contraceptives to thousands of women, many of whom live in “contraceptive deserts,” places where public clinics are difficult to access, CEO Paul Johnson said in an email.
“With challenges to continued funding to Planned Parenthood and other public safety net programs — potential repeal of Obamacare and loss of coverage for contraception — getting access to care easily and reliably will be more important than ever.”
Johnson also sees a big market for women with health insurance as doctor wait times increase across the board.
“Over time, like anything else that is more convenient and accessible, demand will increase,” Johnson said.
“Telecontraception is absolutely a growth market and for good reasons.”
Earlier this year, Portland-headquartered Cambia Health Solutions selected Lemonaid to pilot a new way to get health care for select large-employer groups. A Cambia spokesperson declined to comment on whether contraceptive services are part of the pilot.
Nurx, which launched in 2015, moves into states “where we can make the biggest impact — market size and opportunity, unintended pregnancy rates,” said spokesperson Alex Priest in an email.
Priest declined to speculate when the service would be available in Oregon, where a relatively small proportion of women — 30% —live in a county without an abortion provider, according to the Population Institute, a think tank that ranks states on access to family- planning services (Oregon earned a B- in 2017).
These telecontraception services beg the question: Will digital startups move into abortion services? It’s a murky area, and many companies are hesitant to move into this space. Even in Portland, abortion is a stigmatized practice. Both Kaiser and OHSU declined to make available for interviews physicians who provide abortion services. “It’s too controversial,” says spokesperson Mike Foley, explaining that the health care organization was worried about the safety of doctors who perform abortions.
No federal laws or regulations prohibit mailing of abortion drugs to patients, says Elizabeth Raymond, a researcher who works for Gynuity, the New York-based research organization coordinating the TelAbortion study.
That said, companies that do mail abortion pills are mostly outside the U.S. (For the time being, Lemonaid has no plans to move into “abortifacient” services, Johnson said.) But there is no question that momentum is growing.
The Gynuity project is part of an Investigational New Drug application filed with the FDA. (OHSU, which is part of a national contraceptive clinical network, is also participating in the TelAbortion study.) PPCW recently launched another video abortion pilot called TeleMAB at its Salem, Bend and Northeast Portland health centers.
The program enables a patient at one of the health centers to take the pills while the provider is at another location.
Anti-abortion groups are not languishing on the sidelines. “We’re very concerned about this process of aborting,” Anderson of Oregon Right to Life says. “We’re very concerned informed consent is not taking place. We are also concerned that an unborn child is killed in that process.”
But if these groups view medical and mail-order abortion with alarm, they also consider technological innovation another weapon in the pro-life arsenal.
“Let me go on the record saying that reversing Roe vs. Wade is a long ways away,” Anderson says. But the fact that most new parents use ultrasound as their first baby picture is a boost to the pro life movement, she says. “It’s quite obvious that a human baby is developing.”
No discussion of digital technology and the family-planning divide is complete without examining the explosion in online and mobile applications and vendors. “We’ve been on social media for a long time, but we’re definitely moving all of our platforms to allow folks to use mobile devices,” Anderson says. “We are constantly looking at what tools are available.”
 In a nondescript office building on Northeast Halsey, Larry Gadbaugh, CEO of First Image, a Christian pro-life group, is pushing the organization into the digital age.
In a nondescript office building on Northeast Halsey, Larry Gadbaugh, CEO of First Image, a Christian pro-life group, is pushing the organization into the digital age.
“We have a staff of pretty savvy millennials who keep telling us, ‘You guys are too slow; you have to keep up.’” he says. First Image is working on a phone app to help spread the organization’s message. “It’s one of our priorities,” says Gadbaugh, whose group runs four Pregnancy Resource Centers — clinics that counsel women facing unwanted pregnancy by trying to persuade them to carry their babies to term. They do not offer referrals to abortion providers.
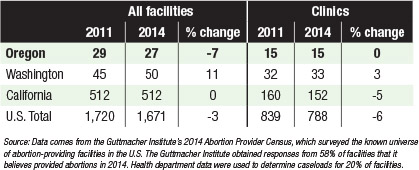 The number of abortion facilities (including hospitals) in Oregon declined between 2011 and 2014, although the number of abortion clinics stayed the same.
The number of abortion facilities (including hospitals) in Oregon declined between 2011 and 2014, although the number of abortion clinics stayed the same.
The nationwide PRC movement got a boost last month, when the Supreme Court California ruling “set a precedent,” Gadbaugh says. “That doesn’t mean the abortion industry can’t attempt some other form of regulation.” PRCs in Oregon — there are around 40 statewide — are not required to offer abortion counseling.
Pro-choice groups like National Abortion Rights Action League (NARAL) post information about services online and do a lot of fundraising using online platforms.
“These technologies allow us to cast a broad net to find supporters and provide a simple way that people can donate directly to care,” says Hannah Rosenau, who serves on the board of the Northwest Abortion Access Fund, a group that raises money for women who want abortions.
But there’s a downside, she says. Two years ago, hackers targeted the abortion access fund’s online abortion fundraiser called the National Abortion Access Bowl-a-Thon. The fund is currently part of a lawsuit against hackers, Rosenau says. The group seek to identify the attackers and hold them accountable for obstructing access to reproductive services.
This fall Oregonians will head for the polls, many largely unaware of how new technologies and the private sector are reshaping access to contraception and abortion. Whether science and tech will tilt the reproductive health landscape in favor of prochoice or anti-abortion policies is unclear.
Digital technologies and on-demand business models have undercut some of the most powerful institutions in the country, in government and business.
But if the changing fortunes — and reputations — of big tech firms like Facebook have taught us anything over the past year, it’s that technology is agnostic, often ruthlessly so. An innovation used to broaden access in one context can just as easily be used to inhibit in another.
“Tech provides an opportunity for women to beat the system,” Udall says. “That doesn’t mean we shouldn’t be fighting really hard to have an administration that supports what the majority of men and women say they want. We have to continue to put policies in place.” Additional reporting by Caleb Diehl.
Sidebar: Male contraception: A pipe dream?
“There are great male hormone methods,” says OHSU’s Jeff Jensen. “They work; they are effective. I’m not optimistic about seeing them.” The logic is convoluted. Basically, female contraception, even if it’s risky (e.g., the pill increases the risk of blood clots), can be viewed as a net health benefit given that pregnancy is inherently dangerous. But the male role in procreation is risk free. So any contraceptive will inevitably heighten the danger for men. “Bayer, Merck — they all had male contraceptive research, and they’ve all stopped them,” says Jensen. That said, biotech startups are moving forward with clinical trials of gels, pills and injections. Demographics could also spur change, as millennial men may be more inclined than previous generations to sign on for a male contraceptive.
To subscribe to Oregon Business, click here.







