As investors flock to the red-hot elder-care market, long-term care bills loom for consumers and Medicaid.
They called her the Norwegian songbird.
A beauty with short brown hair and bright green eyes, she sang at weddings and funerals and had one of the sweetest voices in the choir at the Lutheran Church in Beaverton, a few miles from her home where she raised two children with her husband, the Aloha postmaster.
When he died in 1990, Jenny Tollefsen was only 65. But she was helpless on her own. Though she skied and swam, she spoke broken English and didn’t know how to write a check. Her daughter took over the finances.

Ellen Tollefsen displays a recent photo of her mother, Jenny, who passed away in March. (Photo Shelter)
As the years passed, Tollefsen sunk into the feebleness of old age. She developed dementia and, as often happens, fell and broke her hip. Thus she entered long-term care.
Her daughter got her into a rehabilitation center, Chehalem Health & Rehab in Newberg. She went from there to Brookdale Beaverton, a facility for dementia residents. She ended up at an adult care home, where she died this past March at 93.
Tollefsen was financially fortunate. She had an income of about $4,000 a month from Social Security and her husband’s U.S. Department of Veterans Affairs benefits. Though she was only in long-term care about a year, she burned through her savings and income and then some. Her daughter Ellen Tollefsen had to refinance her own home to pay for her mom’s care.
When her mother died, her room and board and care cost about $8,000 a month. “Money isn’t everything, but it’s certainly a component when you’re trying to keep things going,” says Tollefsen.
Many Oregonians are not prepared for the costs of old age, which can include expensive in-home care and residence in a long-term care facility.For elderly people with chronic conditions who live a long time, the lifetime bill can reach nearly $1 million, according to an analysis by the financial firm, PricewaterhouseCoopers. On average, the study found, Americans who need care later in life pay $172,000 in a lifetime; in Oregon the average is nearly $150,000.
The study was based on claims for long-term care insurance, which covers expenses related to the cost of care. But only a small fraction of consumers even has those policies. “Very few companies are still offering them,” says Larry Rubin, a partner at PricewaterhouseCoopers.
Medicare, the insurance program for seniors, does not pay for long-term care. Medicaid, the insurance program for the poor, does — at soaring costs.
In 2013 the state shelled out about $575 million for long-term care for Oregon Medicaid clients in facilities or adult care homes. In 2017, just four years later, the bill jumped 26% to nearly $730 million due to an increase in the older population, the number of facilities and federal and state rate hikes.
 Touchmark Portland is one of around nine assisted-living facilities slated to open in the metro area in 2018.
Touchmark Portland is one of around nine assisted-living facilities slated to open in the metro area in 2018.
A red-hot market
The outlook for the state — and the consumer — contrasts with the picture for business. The companies investing in elder-care projects reap big profit margins. A percentage in the low 30s is considered decent on a building, says Peter Elwell, a senior-housing specialist at 1031 Crowdfunding LLC, a California-based investment company that just paid $14 million for a Hillsboro memory-care facility, Rosewood Specialty Care.
“There’s a ton of money flowing into the space right now,” Elwell says. “With the silver tsunami — the Baby Boomer generation — coming along that there will be a great need for this product type.”
In 2016 Oregon was home to about 670,000 people 65 and older. About 85,000 of them were at least 85, when people typically need the most care. Flip forward 10 years to 2026 and the number of those 85 and older are likely to increase to more than 100,000 people, according to forecasters at the Oregon Office of Economic Analysis.
With big profits, many private-equity firms and institutional investors are moving into senior housing. The sector is also attracting interest from abroad.
“There’s a lot of foreign money that’s flowed into it, mostly from China,” Elwell says. “When people see a high-performing asset class, they flood it with money and drive up prices. That’s what’s happening.”
Oregon is one of the most popular markets for senior housing, according to the National Investment Center for Seniors Housing and Care, an Annapolis-based nonprofit research group. (Senior housing includes independent-living facilities as well as long-term care communities.)
The Portland metro area ranks sixth out of 99 metro areas for its 93% senior-housing occupancy rate, says Beth Burnham Mace, NIC chief economist. Portland’s 22.7% penetration rate (the percentage of potential customers the industry serves) is more than double the national rate of 11.2%. In other words, 22% of Portland-area seniors live in senior-housing facilities and not at home.
 Waverly Place, an assisted-living and memory-care facility in Albany, opened in February. (Photo Shelter)
Waverly Place, an assisted-living and memory-care facility in Albany, opened in February. (Photo Shelter)
In the past six years, residential care and assisted-living facilities have increased by more than 10% in Oregon. As of the first quarter 2018, there were nine assisted-living projects representing 1,061 units under construction here, according to NIC.
Unlike New York, where most people stay in apartments as they age, “it’s more the lifestyle in Portland,” says Mace. “It’s on the radar for Oregon seniors as they age; it’s on the radar of their adult children.”
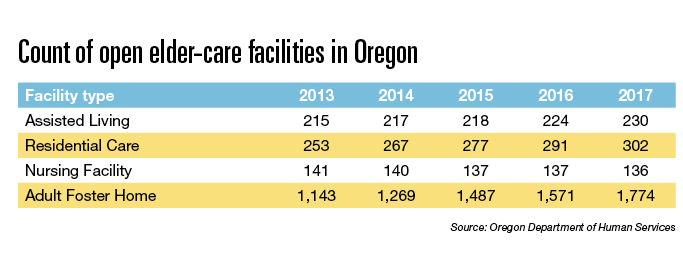
Long-term care innovation fuels demand
The popularity of senior housing in this state dates back to the 1980s, when policymakers started experimenting with long-term care settings. The idea was to house seniors who needed care in an environment that was more like home — not an institutional setting like a nursing home.
In 1981 Oregon became the first state nationwide to apply to the Centers for Medicare & Medicaid for a waiver to use Medicaid dollars to pay for long-term care in settings other than nursing homes. The first licensed assisted-living facility in the country, Rackleff Place, opened in Canby in 1989. Forty percent of the residents were on Medicaid.
Forty years later, long-term care options have proliferated. “There’s been an explosion in the number of large facilities that are operating in the state,” says Rick Davison, former licensing head of adult-care homes for Multnomah County and the longtime director of Adult Living Alternatives, which places the elderly in long-term care. The average assisted-living facility now has about 80 residents, he says.
Adult children, who often select the facility for their parents, prefer the private apartments associated with assisted living, Davison says. And investors have discovered the product yields hefty returns, almost double the return on apartment buildings over the past year.
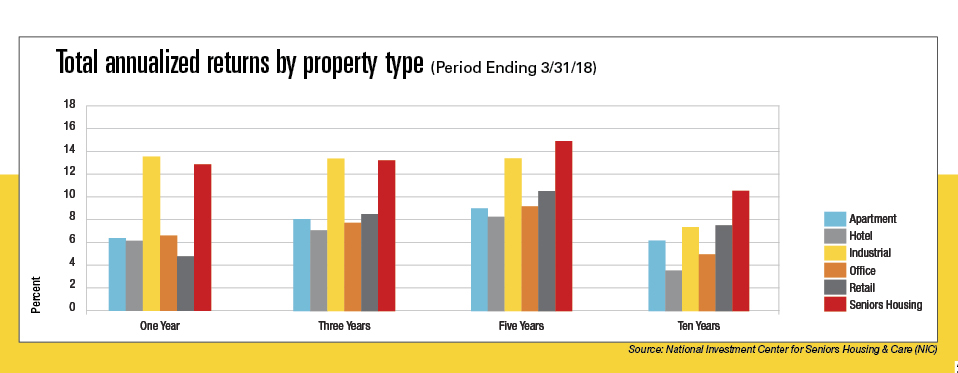
Foreign interest in U.S. senior housing projects started in earnest in 2016, says Lisa Widmier, executive vice president with CBRE’s National Seniors Housing Group. That’s when investors from the Middle East and China, spooked by Brexit and other events, started looking for safe places to park their money.
“The Chinese are also recognizing their own issues with the aging of Chinese people and the need to learn all they can about senior housing business,” Widmier says. “So they come into the United States.” One example among many: In March Shanghai, China-based Fosun International Limited reported a 5.11% stake in Brookdale Senior Living.
Brookdale is one of the largest owners and operators of senior-living communities throughout the United States, operating over 1,000 senior-housing communities in the U.S.
Investor groups say Oregon’s high occupancy and penetration rates mean operators will find more success here than in some other states. According to NIC, Oregon’s assisted-living occupancy rate is 92%.“I personally like Oregon — it’s fiscally pretty sound,” says Elwell of 1031 Crowdfunding. “It’s got a great Medicaid reimbursement rate, and I don’t think it’s overbuilt. The occupancy is pretty high in the whole metropolitan area.”
Independent living has the highest profit margin, he says, because there are no extra service costs or caregivers. Memory-care communities, the fastest growing sector in Oregon, come next. The rooms command a high price, more than regular assisted living and residential care, because residents with dementia need more care, allowing companies to charge for services. The longer people live, the more money the companies make.

The Mirabella Portland, a continuing care retirement community located in the city’s South Waterfront district (Photo Shelter)
Room and board at Rosewood Specialty Care, the Hillsboro memory-care facility Crowdfunding purchased this year, starts at $6,100 for private-pay residents who are relatively independent, but costs go up with added services, like dressing, bathing and toileting. The state pays the facility nearly $3,900 for each Medicaid resident.
Rosewood, like all operators of assisted living, residential-care, memory-care and adult-care homes, decides whether they want to accept Medicaid clients and how many. The state determines who’s qualified based on their needs, assets and income. People who qualify are poor: They can have no more than $2,000 in assets.
The state’s reimbursement rates are substantially less than what people pay when they’re dipping into their own resources. Yet about 80% of assisted-living, residential-care, memory-care and adult-care homes accept Medicaid residents.
That might not seem like a good business plan, but there’s a big upside for the bottom line. Medicaid clients keep facilities full. “It lowers your profit margins,” says Elwell. “But there’s a flip side to it. It helps you fill the beds. So it’s a balancing act.”
“The nursing home industry very strongly lobbies Medicaid for maximum payment,” says Davison. “They are doing very well.”

Brookdale Beaverton, a facility for dementia patients
Workforce challenges
The Rosewood facility is managed by Frontier Management, a long-term care management company that has spread from Oregon to 11 other states. It did not respond to repeated requests for an interview. Brookdale, which operates more than 20 facilities in Oregon, also declined to be interviewed. So did officials at regional companies, including Avamere, Marquis and Pacifica Senior Living. Even executives at small companies were not available.
The long-term care industry can be touchy about interviews. A lot has been written about inadequate staffing and abuse. And nobody wants to reveal profits. According to Elwell, management companies are typically paid 5% of revenues.
About half the revenue from memory care, which can cost $8,000 a month, goes toward paying for staff, Elwell says. About 30% is profit. Much of the rest pays for food, utilities and property costs.
Long-term staff are typically paid minimum wage — about $10 in Oregon. Keeping facilities staffed is a big problem. The jobs can be tough, and the hours vary.
“Workforce challenges are a major concern,” Linda Kirschbaum, head of quality services at the Oregon Health Care Association, the trade group for the for-profit long-term care companies, said in a statement. (She declined to be interviewed.) “The demand for caregivers is projected to grow substantially over the next 10 years due to substantial growth in Oregon’s older population. … With low unemployment rates across Oregon, it will continue to be difficult to fill positions.”
Companies do what they can to attract personnel. A recently opened facility in Southern Oregon that contracts with the state to house difficult Medicaid clients offered a $500 sign-up bonus, half in three months and the rest after six.
“I just hired 60 people,” says Chantele Bangs, owner and administrator of Timber Town Living, a residential-care facility that mainly caters to elderly residents who are difficult to house, she says. All of the residents have “complex behavior problems,” she says. Bangs pays $12 an hour and offers health care benefits, and doesn’t require experience or training — just a caring nature.
“I can train anybody as long as they have the right heart for service.”
A bleak future
There are now nearly 6 million Americans with Alzheimer’s, the most prevalent form of dementia. That’s expected to more than double by 2050. Although the numbers are fueling the elder-care housing boom, there is some concern that overbuilding could put downward pressure on occupancy rates as units come online. To stand out in the crowd, operaters will need to ramp up marketing, even in Oregon, says Mace.
The future looks more bleak on the purchasing side. Experts like Rubin see a long-term-care funding crisis looming for Medicaid. The state — and federal government — does not have the budget now to pay increased costs. Taxes will have to be jacked up and other solutions found. It’s not clear yet what those might be.
The public isn’t prepared either. About one-third of those aged at least 59 don’t have retirement savings or a pension, according to the Government Accountability Office. And about half of Americans only have $10,000 saved for retirement, surveys show. That won’t go far in a long-term-care facility.

Looking ahead, Ellen Tollefsen is worried. She grappled with the expense as her mother slipped away. The bills got paid. But she has no children to lean on when she gets old. Neither does her partner.
“There’s a whole community of us out there,” Tollefsen says. “How everybody is going to manage will be on a wing and a prayer.” (Additional reporting by Linda Baker)
A version of this article appears in the July/August issue of Oregon Business. To subscribe, click here.







